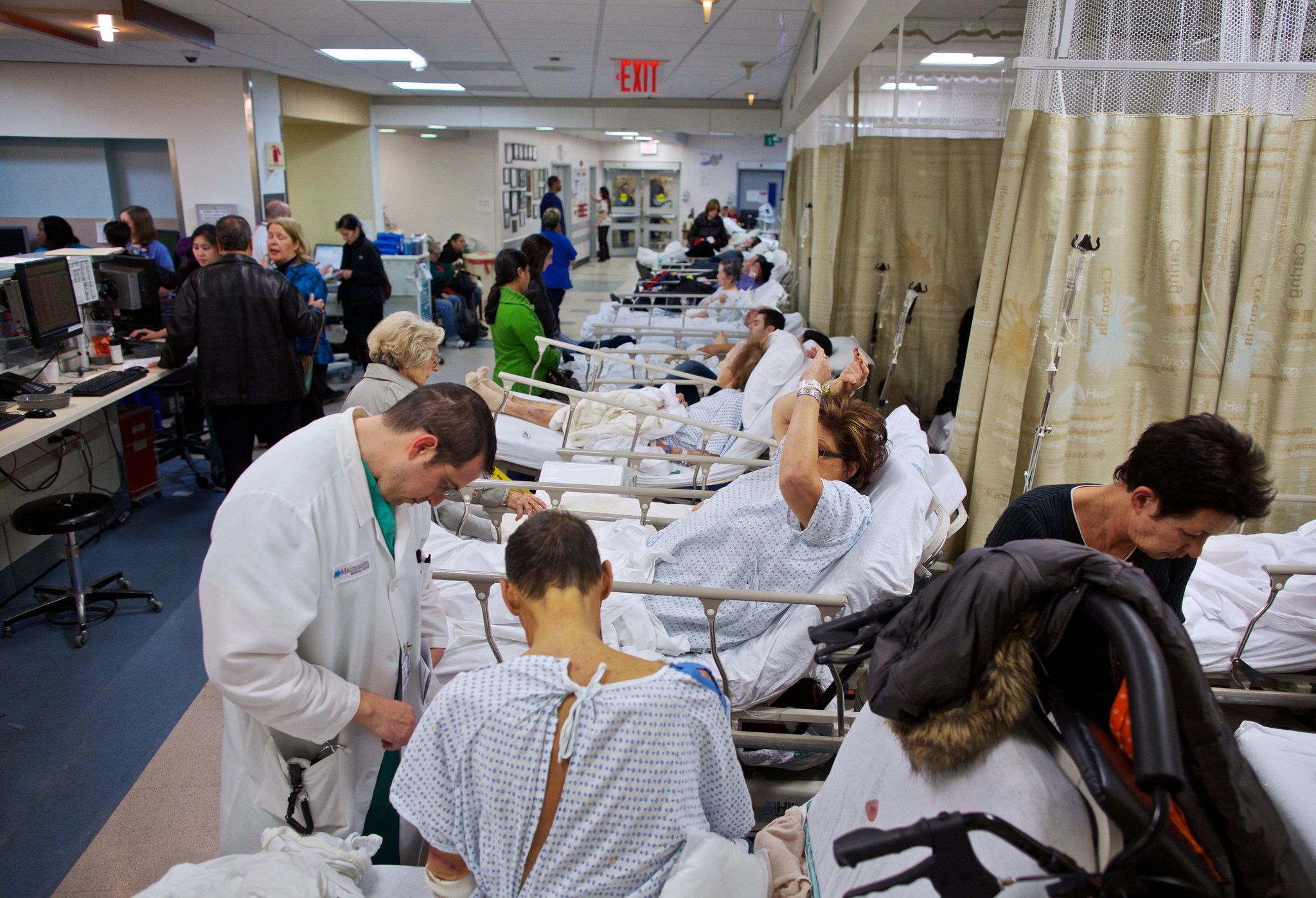
Nurse Ratched Revisited
I awoke in the dark, alone, in pain and frightened. I pushed the call button for the nurse and waited for him to come. Ten minutes seemed like an hour. The pain from my incisions after lung cancer surgery was taking my breath away. When the nurse didn’t come right away I struggled to get out of bed, as the pain was so intense I thought I would vomit. I had no idea my bed had an alarm on it and the alarm started going off – sound and lights. I made my way into the bathroom and was doubled over on the toilet, holding my lung drainage tube up as best I could off the floor when several nursing staff came running in and scolded me for getting out of bed without waiting for them. Looking at the clock on my way into the bathroom I saw that I had gone more than 2 hours beyond the scheduled time to take my pain medication. The nurse stood over me as I sat retching on the toilet and told me in a scolding tone that I was just having a panic attack. He asked if I had them often. I wanted to say that no, only when I had surgery for lung cancer and didn’t get my pain meds on time – but I couldn’t get any words out.
In the following article I’m going to give sometimes scary, sometimes smack-my-head funny and always unbelievable examples of what it’s like to be on the receiving end of a for-profit health care system.
The previously described nurse, who I came to think of as Nurse Ratched, continued to torment me that night. For those of you who don’t remember – “Nurse Ratched is a fictional character and the main antagonist of Ken Kesey’s 1962 novel One Flew Over the Cuckoo’s Nest, as well as the 1975 film. A cold, heartless tyrant, Nurse Ratched has become the stereotype of the nurse as a battleaxe.” (From Wikipedia) When I asked for the stronger pain medication my doctor had promised me I only had to request, Nurse Ratched’s response was, “I have to follow protocol. I first have to give you the milder pain medication, wait to see if that works, and if it doesn’t, only then administer the stronger one.” So there I lay on my bed, rolled into a fetal position, waiting for the 40 minutes to go by before I could get some relief. The only other time I had asked for it -from a different nurse – I received it immediately.
Once the stronger medication was delivered via I.V. and the pain subsided, I was able to think more clearly. When Nurse Ratched came back to check on me I told him I wanted to see a doctor – even though it was 3:00AM. He immediately started to cover his tracks. He told me I was the one who said not to wake me when it was time for my meds. I didn’t try to argue with him – he was clearly in a power position. I didn’t remind him of the conversation my husband and I had with him earlier before he left for the night. To my complaints at being woken up every three hours to take medication, Nurse Ratched had clearly said sympathetically “not on my watch”. Now he kept insisting he wanted to wake me up but was following my orders and this was my own fault. When the doctor finally arrived, Nurse Ratched never left the room. He hovered, making sure I didn’t share that conversation with the doctor or tell him of the nurse’s insensitivity.
Second Surgery
I had been diagnosed with lung cancer just a couple of weeks before my surgery. In an interview with the surgeon before scheduling the surgery, he reassured us that he did this operation all the time and is was a fairly routine procedure. He said I would be in the hospital overnight and go home the next day. We were never told of any risks or complications. When I asked about pain after surgery, he kind of shrugged his shoulders and said that yes, occasionally, people had some nerve pain afterwards, but that was pretty rare and most of the time it went away. He also said that I should be up and about and pretty functional two weeks after the surgery.
When I was settled in my room after my initial surgery and started coming back to my more aware self, I noticed that there was a lot of attention from the staff being given to the tube that came from my lung in order to drain the excess fluid and air into a container that dangled at my bedside. The resident doctor and nurses were checking the tube frequently and conferring with each other. They also seemed to be monitoring my blood pressure and oxygen levels constantly. I didn’t pay much attention to it all because I was still pretty much out of it. It wasn’t until I heard one of them say “60 over 40 – get her back to surgery” and found myself being the center of a drama I had only ever seen in the movies, that I realized I was in trouble. Because my lung was bleeding too much, the need to stop it was urgent. Staff was running down the halls with me on a gurney, swinging me onto a CT scan platform and then, just as quickly, racing back down the halls with me into surgery again. I watched the overhead lights go whizzing past from my prone position.
When they rolled me into surgery and lifted me onto the operating table, I couldn’t believe I was back in this cold, scary room I had left only hours before. I was too weak and frightened to do anything but let the tears roll down my cheeks. I was never given a satisfying answer to my question of what happened to cause the excess bleeding, but have since read that the handling of blood vessels might be related to postoperative bleeding. I can’t help but wonder if the surgeon, who was also overworked, felt rushed or tired as he operated on me. He told me several times after the second surgery that he felt terrible and that it was his fault. As a result of the second surgery I had more complications and a much longer projection of recovery time. I also needed to stay in the hospital for six days and nights, instead of the anticipated one.
The Doctors: One foot Out the Door and One Hand on the Phone
Once in my own room, doctors only came to my room once a day and it appeared that every day there was a different doctor. There seemed to be so many of them I couldn’t keep track. They would come early, 6:30AM or so, while I was still sleeping and too drugged to follow their conversation. Because I was woken up every three hours, I was badly sleep-deprived and managed only catnaps for my entire hospitalization. The doctors would always come when my husband or friend was not there to track and record what they said, ask questions and be my advocate. I wasn’t able to retain whatever they told me – although I tried. They said they would come back later in the day when my husband was there. They never did. Both the doctors and nurses had 2 or 3 cell phones they carried with them, which led to constant interruptions when they were talking to me.
Upon discharge I was released with a three-foot long lung tube with a lung fluid collection box that had to be always kept at least a foot below my lung. A doctor came to my room to teach us how to manage the tube, care for the wounds and drain the blood from the box in which it was collecting. The doctor raced through the procedure, making it hard for all three of us to follow or retain any of it. We also realized – after we got home – that in their rush, they had not provided us with everything we needed to manage on our own. These included tools like the hook to fasten the drainage tube onto the walker, as well as a shoulder strap so I wouldn’t have to hold it in front of me every time I took a step. When we went back to the hospital after discharge to have the tube removed, we learned we had been incorrectly instructed in the proper way to drain the box the blood had been collecting in.
The surgeon never informed us that, even though they successfully got the malignant tumors out, there was a substantial chance the cancer could return, even in other parts of my body. He only discussed the operation as a success; the lymph nodes were clear; there was no sign of cancer anywhere else in my body as it that were the end of the story. It was only 2 weeks later that he informed us that there was only a 30-50% of the cancer not returning in the next five years. This was a complete shock to us and we still are processing it.
The Nurses
Most of the nurses at Kaiser were not like Nurse Ratched. Many of them were supportive, helpful and compassionate, although usually rushed and harried. They were also clearly over-worked. I’ve since learned that if a nurse calls in sick, the other nurses have to pick up the patient load of the sick nurse, making it nearly impossible to give all of their patients the care they need. It was very difficult to build a rapport with a nurse since their rotations were changed frequently and I couldn’t remember all their names. Even though the departing nurse was supposed to come into my room and introduce me to the new nurse, it rarely happened. It’s surprising that I didn’t encounter more bitter, angry, impatient staff like Nurse Ratched.
Nurses operated in a contradictory manner and they expected you to not confront them with the contradictions. Some of them would get upset when you got out of bed without their help, but in most cases they rarely came right away when you called them. At one point a nurse told me to simply wet the bed if I couldn’t wait for them because then they would come in immediately and clean everything up! My surgeon impressed upon me daily the need to get out of bed and walk four times a day to build back my lung function. It was made clear to us that a nurse needed to walk with me, even if my husband was there. But when I asked the nurses to help me walk, they were only able or willing to do it once a day. Finally my husband and I took matters into our own hands and began walking on our own down the halls. The nurses saw us do this and said nothing. We broke the rules and they were complicit. They had to tell us formally to wait for them to walk us, but were secretly relieved we did it on our own. The point of this story is not that there are some good nurses and some bad nurses. Rather, it’s that there is a fundamental unreliability in the whole system. On any given day you don’t know how you will be treated.
Diffused Attention to Patients Under Normal Circumstances
Under normal conditions in the hospital any questions I had that were unique to my condition was treated as cases of “probability”. The staff seemed to think they could not afford to go deep enough to answer my questions that might result from them actually knowing anything about my history. It was only when there was something seriously wrong with me that they focused on me as a person. In other words, I believe they have to stay close to the surface with any patient, so they can slip and slide easily across patients. My guess is that the specter of lawsuits has been deeply impressed on them.
We got constantly conflicting information from different departments. Doctors and nurses would tell us different things about what kind of foods were ok to eat and what to avoid. The nurses told us one way to use the inhaler and the respiratory therapist another way. They would all project different time sequences for recovery. Instead of giving us an average, they would say, “everyone is different”. This concession to bourgeoisie individualism and relativism was trotted out so they wouldn’t have to take a stand and perhaps risk being sued.
Not Being Fully Informed: Tube – What Tube?
When I first realized I had a tube draining fluid from my lungs and that tube would now be a part of me for an undetermined amount of time, I was surprised, creeped out and apprehensive. I had never been told before surgery there would be a tube coming out from between my ribs, so that fact was a shock itself. It was also scary. What would happen if I accidently stepped on it? What if I turned on my side in bed and pulled it out? Why was there so much blood in the tube – is that normal?
Not only did I find out that I would be coming home with a tube in my lung, but also that we were expected to drain the tube and dress the wound ourselves. We were euphemistically told that this was “home care”. Translation: you are on your own. When my husband and I expressed concern and that we needed to see how it was done, both the doctors and nurses raced through the procedure as if watching them do it was the same thing as us learning how to do it. They taught us nothing. We finally, with the support of a good friend who witnessed this, told them we were uncomfortable dealing with an open wound. They did not seem surprised and said we could come back to the hospital to have it done.
“Anti-social Worker”
One day a social worker came in launched into a canned presentation on the five different plans for home care complete with glossy flyers – all of which had costs attached and were privately owned and operated. We asked her if Kaiser would pay for any of these services and she told us she had no idea – we would have to talk to “someone else” in Patient Services. She never once asked us what our actual needs were, nor did she weigh the pros and cons of each one. She also presented this material as if she were at a carnival or a show. There was no sensitivity that I was sleep deprived, on strong pain medication and reeling from the knowledge I had lung cancer and that these rhetorical constraints might indicate that she should go slower. There was absolutely no attempt on her part to read our body language and facial expressions and adjust her presentation accordingly. Nor did she try to help us figure out if we were entitled to any of these services. It was a sales pitch.
What Home Care?
Because we had no knowledge of Kaisers’ home care plans for us, we felt adrift to fend for ourselves and figure out my recovery post-hospital on our own. Even though we asked, we never were able to find out whether we should set something up ourselves, if Kaiser would handle it or if it was even provided. We knew nothing about any of this until we received calls to schedule visits from both the nurse and the physical therapist. It wasn’t until then that we were told our health plan covered the cost. Relieved, we put the piles of brochures from the social worker in a folder.
Home Care Oasis
The difference between the home care and the hospital care was like night and day. A nurse, as well as a physical therapist, came regularly for a month, checking my vital signs and recovery rate and teaching us strengthening exercises and recovery mechanisms. They always stayed for 30 to 45 minutes and answered all our questions in depth. We never felt rushed. We developed a relationship with them and their obvious care and support were such an important part of my recovery. Still we wondered – why in the world weren’t we told we would be provided with this service? It would have relieved us of unnecessary anxiety.
Swarm, Then Disappear
If hospitals were run as rational institutions, the doctors, nurses, respiratory therapists, nursing assistants, food service workers, and social workers would come in one at time – and they would know when the others were coming in. Not at Kaiser. On any given day I had two, three or four in my room at the same time all wanting my attention. Then everyone might disappear for hours. Often when you really needed assistance you couldn’t get anybody to respond to your calls. One afternoon I listened to the woman in the next room feebly calling “nurse, nurse” when no one responded to her call button for well over an hour. I wanted to help her myself but was too weak. All the while she was calling, I saw a nurse or nurse’s aid sitting behind a desk just outside her room. He seemed to pay no attention to her at all, nor did he try to find other staff to help her. Someone told me it was possible she had mental issues. Still, I thought, shouldn’t someone respond to her calls for help?
I learned the hard way that if you don’t have an advocate with you every minute, every hour you’re in the hospital, you’re screwed. I was lucky enough to have a husband who came every day for 8 hours along with a close friend who also would spell my husband. Even with the three of us we barely kept our heads above water. Often the times that required focused attention were when my advocates weren’t there. It’s hard to imagine that an individual with much less support wouldn’t die in the hospital.
The Political Economy of Chemotherapy
The only recommendation after surgery to reduce the chance of a cancer recurrence offered by the oncologist was chemotherapy. I learned, after doing some research on the percentage of success with chemo for my type of lung cancer, that this treatment only had a 5% – 10% chance of it making any difference at all. That low percentage, my age, not wanting to subject my body to poison and the loss of productive, joyful time I would lose if I accepted his recommendation made me decide against it. When I asked if there were any other treatment options he said Kaiser didn’t offer any. I have since read that oncologists get reimbursed from pharmaceutical companies for prescribing chemotherapy. Whether this is true for Kaiser doctors, I have no idea. And yes, there have been laws passed to try to regulate this. However, this is fundamentally an example of capitalism directing choices of healthcare professionals. I hardly think capitalism cares whether we are sick or healthy. When I asked my oncologist about the benefits of choosing a plant-based diet as well as regular exercise, his response was – “it couldn’t hurt”. He then said, “There are no experimental studies that prove it can work”. Fair enough. But what he didn’t say was how much the corporations and drug companies are paying people to write up skeptical studies against alternatives. Or that the cost of doing experimental studies is so expensive that no alternative to chemotherapy has the funding to pay for it.
Conclusion
This may sound like a scene straight out of a horror story like One Flew Over the Cuckoo’s Nest, but all of it is true. The lack of adequate staff to meet the patients’ needs, the misdirected frustration and irritability of the over-worked nurses, the conflicting information we would get from different departments and many more incidents brought home clearly the impact of capitalism on health care. As a matter of fact, my own surgeon told me he needed to get me out of there as soon as possible if I was ever going to recover.
After I was discharged and safely at home, in conversations with my family and friends, I speculated that I received this kind of treatment because it was Kaiser. In fact, I had always joked that Kaiser was great so long as you didn’t have any serious health problems. However, the consistent feedback I got was that it’s like this everywhere with for-profit hospitals, and not just in the U.S. In fact, when I told my surgeon about some of my experiences, he said I was preaching to the choir. He said that’s why he wanted to get me out of there as soon as possible. If we think the hospitals that cater more to the upper middle class are better, like UCSF, we’re mistaken.
The purpose of this writing is not to condemn Kaiser on all fronts. It is to show how erratic capitalist health care institutions are, both within the hospital and between the hospital and home health care. I am pretty close to saying I’d rather risk death than go back to a Kaiser hospital. But so many people have told us that all hospitals are the same. Whenever they are for-profit hospitals, the patients will suffer.
Barbara MacLean has worked as an academic and career counselor at California State University, East Bay and as a career counselor and manager of the downtown Oakland One Stop Career Center, a public career and jobs center in partnership with EDD. She is a socialist feminist. She is a founder and organizer for Planning Beyond Capitalism. Follow them on Facebook and Twitter Email her at mailto:barbaramaclean8@gmail.com